Basic Introduction to Cytogenetics
Cytogenetics is the branch of genetics that studies the structure and behaviour of chromosomes and their relation to human disease and disease processes.
Cytogenetic studies show the significant contribution of chromosome aberrations to infertility, pregnancy loss at all stages of gestation, and developmental disabilities and congenital malformations in the newborn. The study of human chromosomes also contributed to the understanding of the relation of genetics to the origin of cancers, the physical mapping of genes, and the prevention of genetic diseases by prenatal testing.
Specimen preparation varies with the type of tissue undergoing chromosome analysis. In most instances, the tissues are cultured in a synthetic media to increase the number of cells in mitosis available for cytogenetic analysis. After the culturing, the specimen undergoes a process of harvesting and staining in preparation for microscopic examination of the chromosomes. The time required to complete the chromosomal analysis varies with the type of tissue.
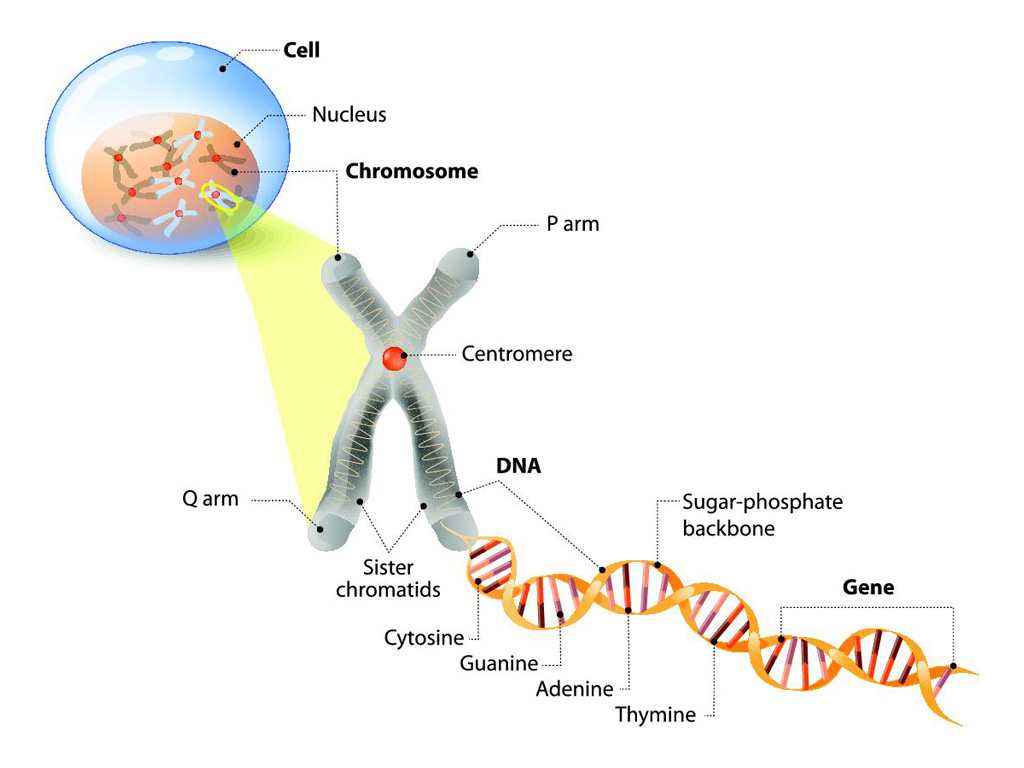
One complete set of human chromosomes consists of 23 chromosomes. A complete set is referred to as the haploid number (N); for humans, N = 23. A normal human somatic cell contains two complete sets of chromosomes, one of maternal origin and the other of paternal origin. There are 46 chromosomes in the nuclei of all human somatic cells; this number is known as the diploid number (2N); for humans, 2N = 46.
Chromosomes are classified as autosomes or as sex chromosomes. There are 22 autosomes in the human chromosome complement. Because a somatic cell contains two members of each chromosome, there are 22 homologous (morphologically similar) pairs in human cells. Cells with two X chromosomes are classified as female, and cells with one X and one Y chromosome are classified as male. These two chromosomes are the sex chromosomes.
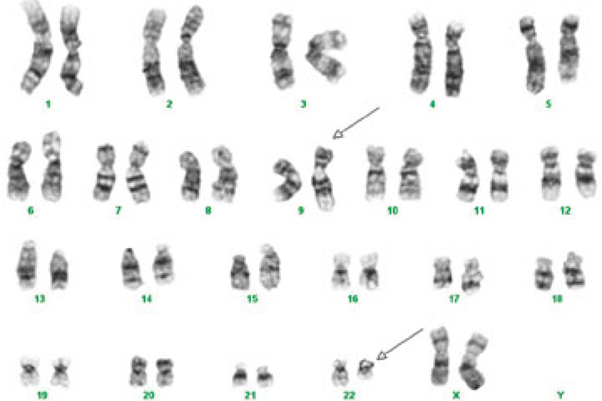
A routine cytogenetic analysis involves evaluating cells to determine their modal chromosome number and assessing the structural integrity of each chromosome in the complement. Identification of an extra or missing chromosome is possible by microscopic examination, and the finding is confirmed through the preparation of a set of karyotypes. A karyotype is a photographic or computer-generated representation of the chromosomes in a cell arranged according to size, centromeric position, and banding pattern. Assessment of the structural integrity of each chromosome in the complement can also be made through the microscope, and gross structural chromosome aberrations can be detected as well.
Chromosomal analysis can be performed on cells derived from many sources, including peripheral blood lymphocytes, fetal blood, chorionic villi, amniotic fluid cells, skin and bone marrow.